Resources
VITALCORE STAFF ARE OUR HEROES
The COVID-19 pandemic has placed a huge burden on medical staff throughout the United States which has resulted in staff shortages. VitalCore’s employees have continuously cared for all patients, including those affected by COVID-19 and have managed the complexities of screenings and quarantining. The work has never been harder, yet our staff has remained dedicated to providing quality healthcare.
WE APPRECIATE YOU!

OUR COVID-19
Pandemic Planning Team

Beginning in March 2020, VitalCore established a COVID-19 Pandemic Planning Team that has met weekly ever since. This multidisciplinary team includes the Chief Operating Officer for Clinical Affairs, Senior Vice President for Nursing, the Regional Medical Directors, in addition to other national expert consultants in correctional infection control.
At our weekly Pandemic Meetings, data on new cases and outbreaks are reviewed to develop guidance on best practices for response. Updated CDC guidance and pandemic news is discussed. Revisions to our VitalCore COVID-19 Pandemic Response Plan are reviewed and approved.
VITALCORE Pandemic Response Plan
Prior to Centers for Disease Control and Prevention (CDC) developing guidance for COVID-19 correctional facilities, VitalCore developed a robust plan which was shared widely in the correctional world. The VitalCore COVID-19 Pandemic Response Plan is updated regularly reflecting the latest guidance from CDC and evidence-based medicine. The VCHS pandemic response plan includes:
Administration/ Coordination/ Communication
Intake Screenings
Cohorting of Intakes
Personal Protective Equipment (PPE)
Isolation and Treatment of Cases of COVID-19
Quarantine of Persons Exposed to COVID-19
COVID-19 Testing Recommendations
Health Care Delivery during COVID-19
Prior to Centers for Disease Control and Prevention (CDC) developing guidance for COVID-19 correctional facilities, VitalCore developed a robust plan which was shared widely in the correctional world. The VitalCore COVID-19 Pandemic Response Plan is updated regularly reflecting the latest guidance from CDC and evidence-based medicine. The VCHS pandemic response plan includes:
Administration/ Coordination/ Communication
Intake Screenings
Cohorting of Intakes
Personal Protective Equipment (PPE)
Isolation and Treatment of Cases of COVID-19
Quarantine of Persons Exposed to COVID-19
COVID-19 Testing Recommendations
Health Care Delivery during COVID-19
Mitigating the health risks of COVID-19 has been an unprecedented challenge for correctional facilities. From the beginning of the pandemic, VitalCore has implemented comprehensive infection prevention and control plans to contain COVID-19 and to promote the health and well-being of our health care professionals and incarcerated patient populations. VitalCore recommends that incarcerated persons be vaccinated against COVID-19 if their length of stay allows for it. We have had extraordinary success vaccinating incarcerated persons in our two prison systems with long lengths of stay: Vermont DOC and Mississippi DOC.
HOW COVID-19 SPREADS
SARS-CoV-2 (the virus that causes COVID-19) spreads when an infected person breathes out droplets and very small particles that contain the virus. These droplets and particles can be breathed in by other people or land on their eyes, noses, or mouth. In some circumstances, they may contaminate surfaces they touch. People who are closer than 6 feet from the infected person are most likely to get infected.
COVID-19 is spread in three main ways:
- Breathing in air when close to an infected person who is exhaling small droplets and particles that contain the virus.
- Having these small droplets and particles that contain virus land on the eyes, nose, or mouth, especially through splashes and sprays like a cough or sneeze.
- Touching eyes, nose, or mouth with hands that have the virus on them. (Centers for Disease Control & Prevention)
RISK FACTORS
Close contact with a person who has COVID-19, living in or traveling in place with sustained community transmission. In addition, the CDC has indicated that certain populations may be at a higher risk of developing more serious complications such as older adults, those with diabetes, lung disease or underlying medical conditions.
TYPICAL SYMPTOMS
It is possible to be infected with SARS-CoV-2 (the virus that causes COVID-19) and not develop any symptoms. People can have a range of symptoms, from mild to severe, and may include but not be limited to fever, chills, shortness of breath/difficulty breathing, cough, sore throat, congestion/runny nose, new loss of taste or smell, muscle or body aches, fatigue, headache, diarrhea, nausea or vomiting. The list of symptoms may change with mutations of the virus; refer to CDC.
EMERGENCY WARNING SIGNS
Seek medical attention immediately if you experience:
- Trouble breathing
- Persistent pain or pressure in the chest
- New confusion
- Inability to wake or stay awake
- Pale, gray, or blue-colored skin, lips, or nail beds, depending on skin tone
Note: If you have a medical emergency and need to call 911, notify the operator that you have or think you might have COVID-19. If possible, put on a facemask before medical help arrives or inform them you don’t have a mask.

QUARANTINE
Quarantine when you might have been exposed to the virus and may or may not have been infected.
ISOLATION
You isolate when you have been infected with the virus, even if you don’t have symptoms.
DISCONTINUING
Discontinuing quarantine and/or isolation should be based on recommendations from your local health department or healthcare provider. Refer to the CDC website for information regarding quarantine and isolation guidelines.
HOW TO PROTECT YOURSELF & OTHERS
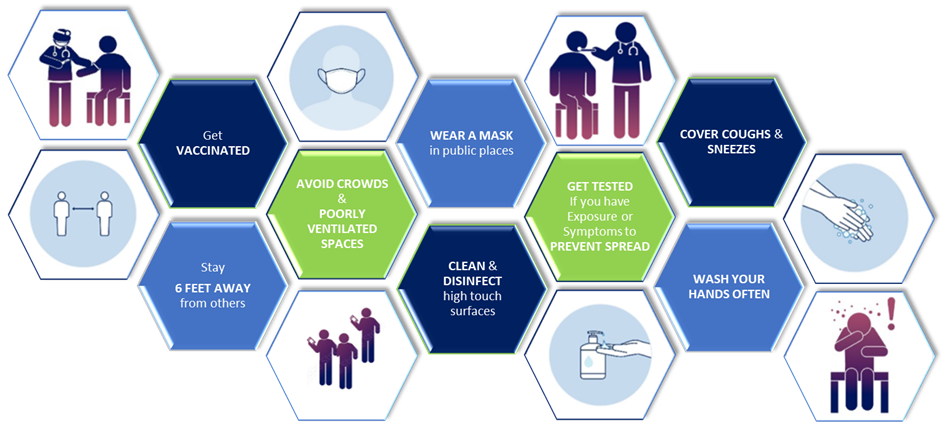
Refer to the CDC website for a full description of recommendations. Our COVID-19 response plan is based on guidance from the CDC, state and local public health authorities, and input from national experts. We remain steadfastly committed towards fighting this pandemic with all available resources.
Selected RESOURCES
COVID-19
CDC RESOURCES
The CDC COVID-19 website provides a wide array of resources that VitalCore has used to develop its policies and procedures related to COVID-19. Below are annotated links that we have found particularly useful.
Resources for Correctional & Detention Facilities. This site provides general resources for people who work and reside in prisons, jails, and detention centers.
- Interim Guidance on Management of COVID-19 in Correctional & Detention Facilities. This is the go-to document that provides a comprehensive overview of infection prevention and control guidance for correctional facilities.
- Print Resources for Correctional and Detention Facilities. Provides print-only materials to support COVID-19 recommendations that are free to download and may be printed on a standard office printer.
Infection Control Guidance. Provides comprehensive guidance on general COVID-19 infection control.
COVID-19 Vaccination: Detailed clinical resources for each COVID-19 vaccine are provided including links to the Emergency Use Authorizations, ACIP recommendations, storage and handling, vaccine administration, and training and education.
Vaccinate with Confidence: Provides materials for health care professionals to reinforce confidence in COVID-19 vaccines.
COVID-19 Data Tracker. Provides a detailed overview of COVID-19 at the county level including the COVID-19 case rate, percent positivity on COVID-19 tests and the percentage of the population fully vaccinated.


EMOTIONAL SUPPORT, SAFETY & RECOVERY RESOURCES
If you have increased worry or despair, know you are not alone. Please reach out for support. There are many mental health professionals across the Nation currently offering free support and resources to people in their communities. Research for resources online by searching “mental health therapists offering free services during COVID-19 near…” then enter your city or zip code. Be sure to explore what services are offered through your county’s Mental Health Centers, Health Departments, Community Service Agencies, etc. In addition, please refer to the National resources listed below.
Note: none of these resources are affiliated with VitalCore or any of the facilities.
- Find a Therapist/Counselor or other resources search: www.psychologytoday.com
- Psych Central for MH resources and online support search: www.psychcentral.com
- Multiple Crisis Resources search:
https://suicidepreventionlifeline.org/talk-to-someone-now/
- Various types of resources and support: search “National Alliance on Mental Illness (NAMI): https://www.nami.org/Support-Education/Support-Groups
- Free online text chat for emotional support and counseling also offered in Spanish: https://www.7cups.com/
- Emotions Anonymous: www.emotionsanonymous.org
- Virtual support groups on numerous mental health conditions – free or low-cost also offered in Spanish: www.supportgroupscentral.com
- Free online peer support groups for mental health challenges and/or difficult family dynamics a safe place to connect. Support groups include Addiction, Anxiety, Depression, HIV/AIDS, LGBT, Marriage/Family, OCD and Teens: www.support.therapytribe.com
https://suicidepreventionlifeline.org/talk-to-someone-now/
- Various types of resources and support: search “National Alliance on Mental Illness (NAMI): https://www.nami.org/Support-Education/Support-Groups
- Free online text chat for emotional support and counseling also offered in Spanish: https://www.7cups.com/
- Emotions Anonymous: www.emotionsanonymous.org
- Virtual support groups on numerous mental health conditions – free or low-cost also offered in Spanish: www.supportgroupscentral.com
- Free online peer support groups for mental health challenges and/or difficult family dynamics a safe place to connect. Support groups include Addiction, Anxiety, Depression, HIV/AIDS, LGBT, Marriage/Family, OCD and Teens: www.support.therapytribe.com
National Safety
Hotlines
Most are available 24/7
National Suicide & Crisis Lifeline:
Dial or Text “988”
(SPANISH) Nacional de Prevención del Suicidio:
Dial or Text “988”
(Hearing Impaired): Dial or Text “988”
(Veterans Crisis Line): Dial or Text “988”
Disaster Distress Helpline: 1-800-985-5990
[National Alliance on Mental Illness (NAMI): M-F (10-6)
Dial or Text “988”
(Veterans Crisis Line):
1-888-628-9454
(Hearing Impaired): 1-800-799-4889
(Veterans Crisis Line): 1-800-273-8255
Disaster Distress Helpline: 1-800-985-5990
[National Alliance on Mental Illness (NAMI): M-F (10-6)
1-888-628-9454
(Hearing Impaired): 1-800-799-4889
(Veterans Crisis Line): 1-800-273-8255
Disaster Distress Helpline: 1-800-985-5990
[National Alliance on Mental Illness (NAMI): M-F (10-6)
1-800-950-6264
Texting
Support Lines
(Crisis Support Text Line 24/7):
Text 988 or “HOME” to 741-741
(Veterans Crisis Text Line): Text 988 or 838988
(Disaster Distress Text Helpline):
Text “TalkWithUs” to 66746
12-Step and/or
Recovery

